 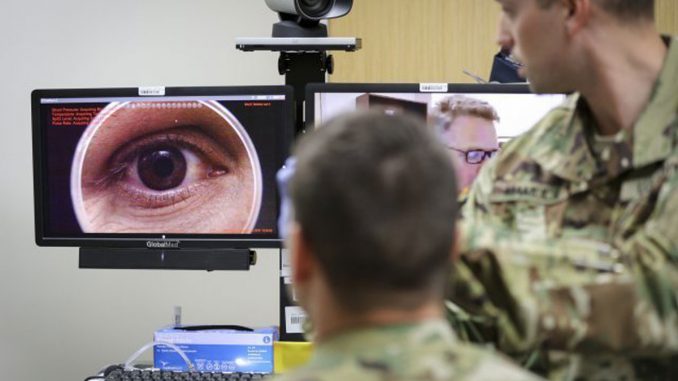
The office charged the whole visit - $280, not just the copay ― to his debit card without notifying him. "So these providers are protecting themselves upfront by either asking for full payment or by getting the copayment."ĭavid DeKeyser, a marketing strategist in Brooklyn, N.Y., sought a physician's advice via video after coming in contact with someone who attended an event where coronavirus was detected. "A lot of providers may not have agreements in place with the plans that they work with to deliver services via telemedicine," she says. New rules notwithstanding, many practices may be eager to collect telehealth revenue immediately from patients rather than wait for insurance companies to pay, says Sabrina Corlette, a research professor and co-director of the Center on Health Insurance Reforms at Georgetown University. Many employer plans are starting to eliminate cost sharing, such as copays and deductibles, now that federal regulators have eased the rules for certain kinds of plans to improve telehealth benefits, says Brian Marcotte, CEO of the National Business Group on Health, a coalition of very large, mostly self-insured employers.įor many doctors, business and billings have plunged because of the coronavirus shutdown. Shots - Health News Psychiatrists Lean Hard On Teletherapy To Reach Isolated Patients In Emotional Pain "A lot of the insurers who said that they're not going to charge copayments for telemedicine ― they haven't implemented that," says George Favvas, CEO of Circle Medical, a San Francisco company that delivers family medicine and other primary care via livestream. Executives at telehealth organizations say insurers have been slow to update their software and policies. Patients say doctors and insurers are charging them upfront for video appointments and phone calls - and not just copays but sometimes the entire cost of the visit, even if it's covered by insurance.ĭespite what politicians have promised, insurers said they were not able to immediately eliminate telehealth copays for millions of members who carry their cards but receive coverage through self-insured employers. In some cases, doctors are billing for telephone calls that used to be free. Andrew Cuomo said last month after ordering insurers to eliminate copays, which are typically collected from the patient at the time of a doctor visit, for telehealth sessions.īut in a fragmented health system - which encompasses dozens of insurers, 50 state regulators and thousands of independent doctor practices ― the shift to cost-free telemedicine for patients is going far less smoothly than the speeches and press releases suggest. "We are encouraging people to use telemedicine," New York Gov. Policymakers and insurers across the United States say they are eliminating copayments, deductibles and other barriers to telemedicine for patients confined at home who need to consult a doctor for any reason. But "they said, 'No, it goes toward your deductible and you've got to pay the whole $70,' " she says. So Taylor, a sales manager, talked with her physician on an Internet video call. The number of COVID-19 cases had just exceeded 5,000 in Texas, where she lives.Ĭigna, her health insurer, said it would waive out-of-pocket costs for telehealth patients seeking coronavirus screening through video conferences. Karen Taylor had been coughing for weeks when she decided to see a doctor in early April. Despite recent changes in insurance policy, some patients say doctors and insurers are charging them upfront for video appointments and phone calls - not just copays but sometimes the entire cost of the visit, even if it's covered by insurance.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
